Shellfish poisoning risk on the rise
We love our shellfish in California, but this spring we’re serving up a warning. Dangerous levels of paralytic shellfish toxin (PSP) have been detected off our Northern coasts. The California Department of Public Health has issued health advisories alerting people not to eat mussels, clams, oysters, or scallops that are recreationally harvested from Del Norte, Sonoma, Marin, and San Mateo counties.
CDPH has also issued its annual blanket quarantine on all recreationally harvested mussels statewide, effective May 1 through October 31, 2026, spanning the coastline from Oregon to Mexico.
Commercially sold shellfish remain safe to consume.
Shellfish advisories in effect, California coast
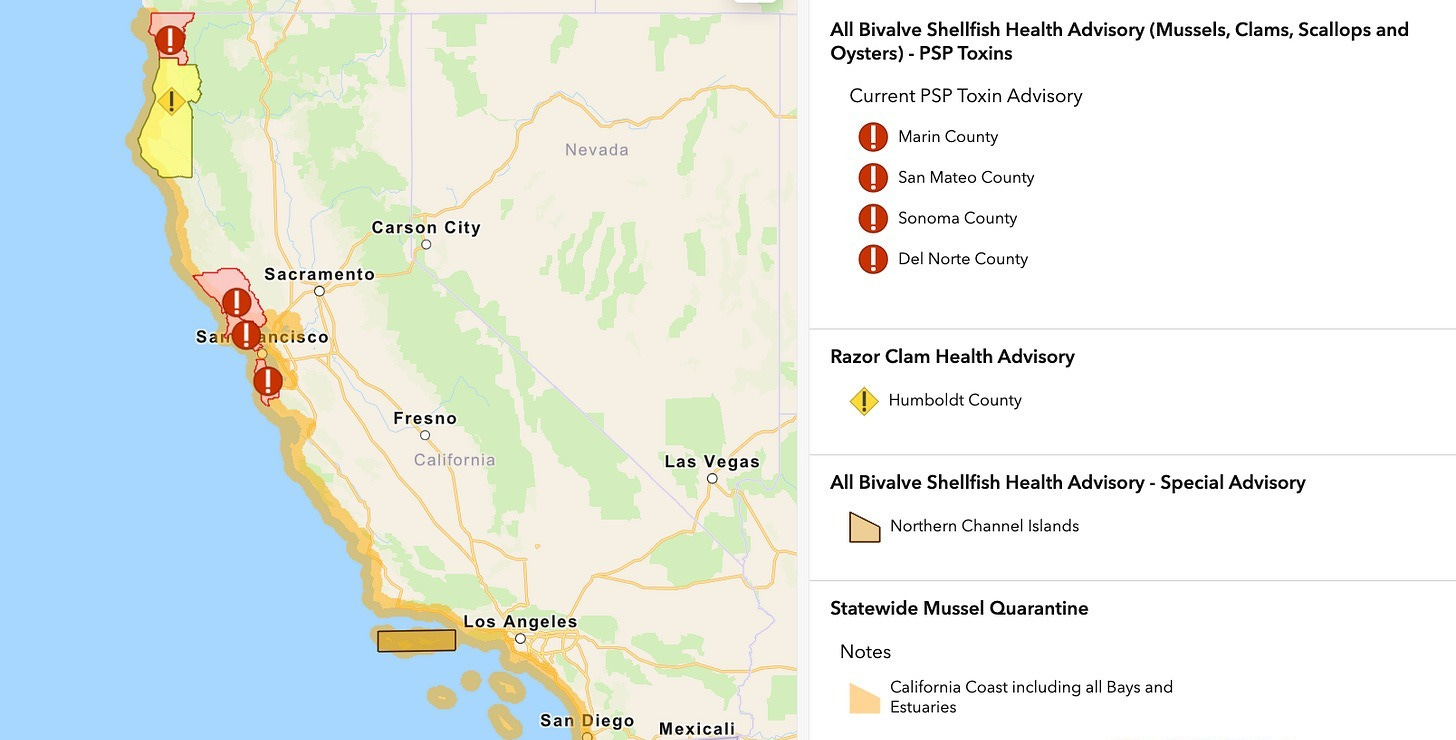
What Is PSP? Paralytic shellfish poisoning is caused by saxitoxin, a potent neurotoxin found in shellfish during harmful algal blooms. When consumed, saxitoxin prevents nerve signals from transmitting across the nervous, respiratory, cardiovascular, and digestive systems, causing paralysis.
Shellfish concentrate saxitoxin by filter-feeding on certain algae. Importantly, cooking doesn’t destroy the toxin, and there is no color, taste, or smell to warn you.
Early symptoms include tingling and numbness of the lips and tongue, which can begin within minutes to a few hours of eating toxic shellfish, followed by loss of balance, slurred speech, and difficulty swallowing. Severe cases can be fatal, when breathing muscles are paralyzed. There is no antidote; treatment is supportive, and keeping people ventilated if needed until the toxin passes through their system. Survivors generally recover within a few days.
PSP in California. The state’s monitoring system goes back to a 1927 outbreak on the San Francisco coast, when 102 cases were reported, including six deaths, prompting PSP to become a mandatorily reportable condition in California. Since then, at least 582 cases, including 39 deaths, have been attributed to PSP in California.
A warming ocean is making this worse. PSP risk is another hidden health impact of climate change. As ocean temperatures rise, harmful blooms of algae that carry saxitoxin are intensifying and lasting longer.
Global Ocean Heat Content, 1958-2025
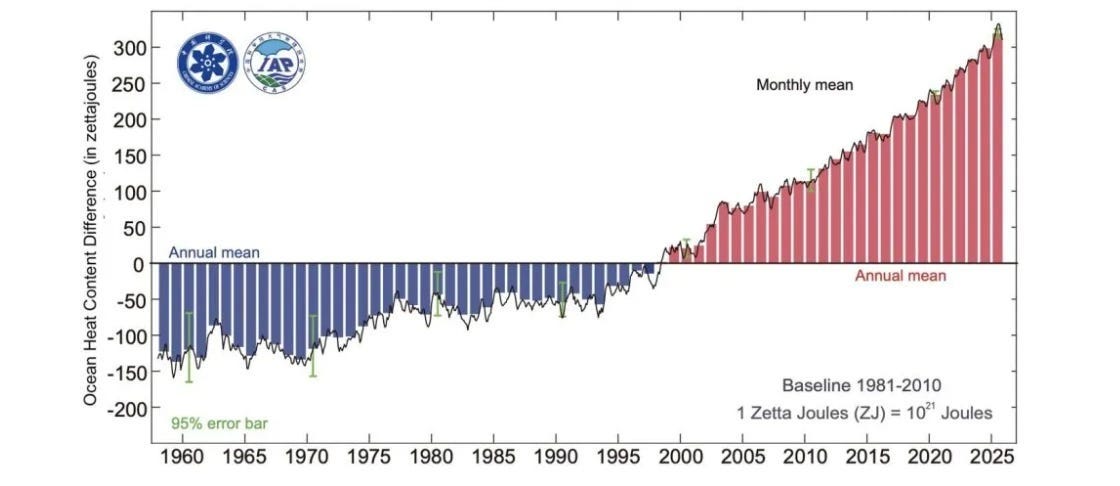
Human cases appear to be following. The strongest surveillance data comes from British Columbia, where records go back to 1941. They found a significant increase in cases that correlated to rising ocean temperature.

California’s coastal monitoring system. CDPH’s Marine Biotoxin Monitoring Program operates a statewide network to collect and test samples from shellfish year-round. Collection sites are stretched across more than 840 miles of coastline. Volunteers up and down the coast help collect samples.
Since 2013, the Tolowa Dee-ni’ Nation—the original peoples of Del Norte County—has been submitting shellfish samples from their ancestral coastline to CDPH analysis. This partnership is a continuation of indigenous coastal knowledge that predates the state by centuries. Recent samples containing PSP triggered the current advisory for Del Norte County.
Preventing PSP:
Don’t eat mussels recreationally harvested from anywhere on our coast from May 1 to October 31.
Don’t eat any shellfish recreationally harvested from San Mateo, Marin, Sonoma or Del Norte county until the current advisory is lifted.
Call CDPH’s Biotoxin Hotline at (800) 553-4133 before harvesting any shellfish—advisories can extend outside the quarantine window or emerge within hours.
Commercially sold shellfish are safe. Licensed harvesters are subject to mandatory testing and are not covered by the quarantine.
If consuming clams or scallops, remove and discard the digestive organs and any dark parts, eating only the white meat.
If symptoms develop after eating shellfish, seek emergency care immediately.
If you live along the coast and want to be part of the volunteer shellfish monitoring network, contact CDPH at redtide@cdph.ca.gov or call (800) 553-4133.
Using paperwork to reduce public benefits
There’s a quiet strategy running through federal policy that will reduce access to food and health care for low income Californians. It hasn’t received a lot of attention, but it reflects a deeper federal agenda to undermine support for our most vulnerable residents.
Access to nutrition: Starting June 1, 2026, recipients of CalFresh recipients—California’s version of federal food assistance—will face new work reporting requirements. Adults without children will have to document at least 20 hours per week of work, training, or community service, or lose food benefits after three months.
Access to healthcare: Starting January 1, 2027, adult enrollees in Medi-Cal—California’s Medicaid health insurance program—will have to meet new work requirements and re-prove their eligibility every six months, instead of annually. A missed deadline could mean losing health coverage.
The stated reason by federal leaders is fiscal discipline. On the surface, these may sound like reasonable measures to ensure only people who are eligible, and are taking steps toward employment, are receiving public benefits.
I saw firsthand what these policies will actually mean when I worked as a primary care doctor in community clinics. For working people, caregivers, and people managing chronic illness, spending a weekday afternoon at a county office, with repeat visits, isn’t just an inconvenience. It’s unrealistic and unkind, and some eligible people will lose health care or food assistance.
The evidence base: Good policy, like good science, relies on evidence. Research consistently shows that when new tasks are added to stay enrolled in services, those who are filtered out aren’t people who are ineligible. It’s mostly people who are eligible but overwhelmed.
The data are clear:
When Medicaid redeterminations were eliminated during the Covid pandemic, enrollment among eligible families rose 30%. When they were reinstated, 73% of disenrollments were among people who were eligible, but didn’t navigate the paperwork.
When states imposed work reporting requirements for food assistance, caseload reductions of 40–60% were documented in Kansas and Oklahoma, and 80% in Maine—not because people found jobs, but because they lost benefits.
The Congressional Budget Office estimated that expanded work requirements would reduce SNAP enrollment by over 3.2 million adults nationally.
The hidden cost: inefficiency and churn. When someone loses Medi-Cal because they missed a deadline, they often return to re-enroll in the program weeks or months later—once they’ve gone without care, or shown up in an emergency room without insurance. Each exit and re-entry generates a fresh round of administrative work.
In health policy lingo, this is called churn. Churn-related administrative costs run to hundreds of millions of dollars annually across state Medicaid program—money spent not on care, but on red tape, processing the same eligible people in and out of the system. With high churn, we spend more to serve fewer people.
California can’t fully shield its residents from these new federal mandates, but it can work to implement them with maximum support, clear outreach, and streamlined processes. The impact of these policies will be monitored closely as they roll out. Good data will allow the necessary course corrections for future administrations.
What you can do: If you or someone you know receives Medi-Cal or CalFresh, there are steps you can take now to protect access to benefits.
First, know your renewal dates and update your contact information. Many people lose benefits because a renewal notice went to an old address or a deadline passed unnoticed. Make sure your county has your current phone number, mailing address, and email.
BenefitsCal.com: California’s unified online portal to apply for, renew, and manage Medi-Cal, CalFresh, and CalWORKs in one place. You can upload documents, check your renewal date, and respond to requests without visiting an office.
Covered California: If you lose Medi-Cal eligibility, Covered California is your next stop. Losing Medi-Cal qualifies as a life event that opens a special enrollment window—don’t wait.
California Department of Social Services (CDSS): The state agency administering CalFresh. Their site includes updated guidance on the work requirements taking effect June 2026, exemption criteria, and how to appeal a termination.
If you need help navigating the process, community organizations across California offer free enrollment and renewal assistance. Search findhelp.org by zip code for local navigators, food banks, and legal aid offices that specialize in public benefits. Many offer same-day help.
Hantavirus: One more Californian being monitored, and no cases
On Tuesday I covered the Andes virus situation in California in detail. (Catch up here.) Here’s where things stand currently.
The main change since Tuesday is an additional passenger has been identified as a California resident and is also in quarantine. The passenger disembarked before the outbreak was recognized and traveled to an island in the Pacific via California. Monitoring is taking place there.
A total of five California residents are now being monitored: one in Santa Clara County, one in Sacramento, two in federal quarantine in Nebraska, and now one on Pitcairn Island in Polynesia. All are doing well with no sign of infection.
An unfamiliar, deadly virus on a cruise ship is bringing back memories for us in California, but Andes virus is not Covid. It doesn’t spread easily, and public health teams are watching even potential cases closely. There are no cases of Andes hantavirus disease in California. Our risk remains very low.
Bottom line
This week’s health news highlights our dependence on hidden public health systems. Coastal monitoring catches toxins before they reach our dinner plates. Streamlined benefits keep people fed and insured. Outbreak control systems track people exposed to a virus on the other side of the world. We trust our policymakers are taking note— each only works if it’s well supported. If we take them for granted, they may disappear.
I’ll be taking next week off. Katelyn from YLE National will pinch hit if there’s anything urgent to communicate. Be well, and see you late May.
Love,
Matt
Dr. Matt Willis is the author of Your Local Epidemiologist in California. A California native, he’s served as a primary care physician, CDC epidemiologist, and public health officer for Marin County, where he guided the pandemic response. He lives in Marin with his family and their dogs Teddy and Ramona.



Just want to tell you again how much I enjoy your weekly information. Easy to understand, important information....but told as if being given to a friend. THANK YOU
I’m sharing this information with our local mutual aid group. What source do I list? Your local epidemiologist? Do we have a website or such to direct people to?